MY VASCULAR HEALTH
Aortic Dissection

Overview
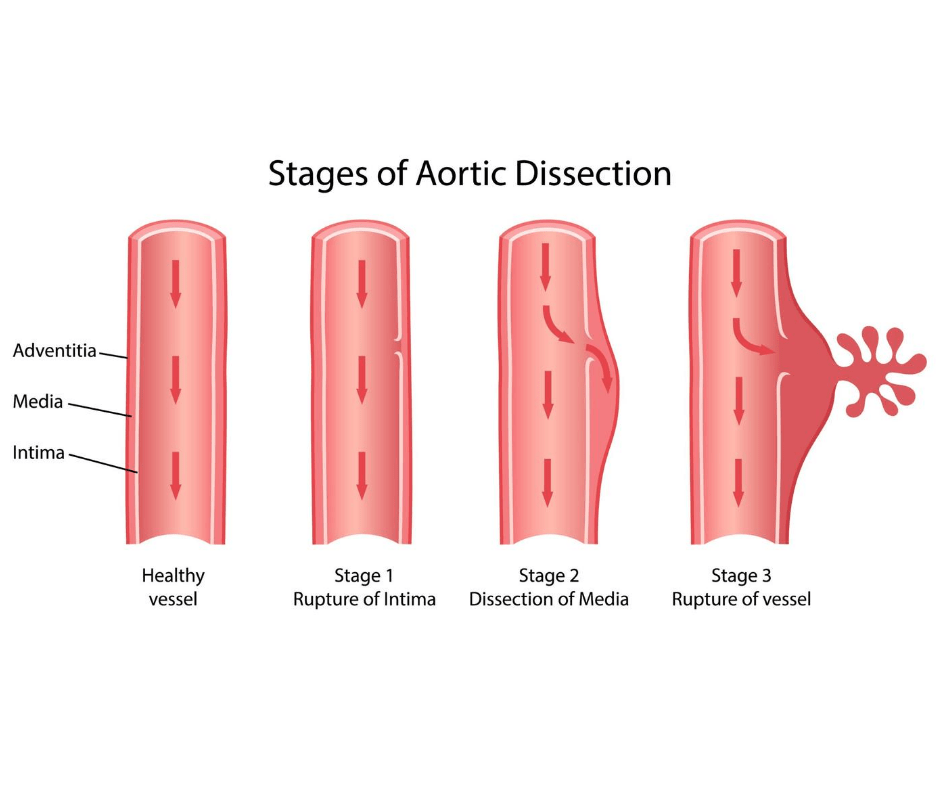
Aortic dissections are one of the most catastrophic and life-threatening events affecting the aorta; this condition brings tens of thousands of Americans to the emergency room each year. In a vast majority of cases, uncontrolled hypertension causes a tear in the aortic wall. This tear results in forceful blood flow within the newly created false lumen, which competes with the original or true lumen and results in a weakened aortic wall. Once the tear has begun, the high blood pressure will continue to perfuse the false lumen and expand this dissection. Depending on the site of the aortic tear, the damage can go on to involve the heart vessels and the valves, and if it propagates forward, the tear can affect other major branches of the aorta that perfuse the abdominal organs and lower extremities. As the false lumen expands, the blood supply through the true lumen can become choked off, resulting in organ malperfusion and complications including stroke, heart attack, congestive heart failure, kidney failure, paraplegia, and limb-threatening ischemia.
The majority of patients are between the ages of 50-80 years, although younger patients with hypertension or connective tissue disease are also at risk. Patients describe the pain associated with acute aortic dissection as “sharp” and “tearing,” often located in the chest and between the shoulder blades and can mimic symptoms of a heart attack.
Signs & Symptoms:
- You may experience no symptoms and learn you have an aortic dissection in the process of being tested for other reasons.
- If you have a known aortic dissection and you experience chest/back pain, you need to consider going to the nearest emergency room and contacting your doctor immediately.
Treatment Options:
Once aortic dissection is diagnosed, immediate medical treatment includes the use of anti-hypertensive drugs, and vascular surgery, and possibly cardiac surgery consultation. The optimal management is directed toward identifying whether an aortic dissection is complicated or uncomplicated. Patients with complicated dissections present with organ malperfusion, refractory pain, or rupture, and they require immediate surgical or endovascular treatment. For a vast majority of patients in whom the aortic tear occurs in the descending thoracic aorta, endovascular repair is considered the “gold standard.” In patients with ascending thoracic involvement, surgical repair is preferred.